
Onychomycosis is a widespread (up to 18% of the population) fungal nail disease. It affects people of all ages, and an increase in the number of affected people in the past decade has also been noted among adolescents and children. Due to the high contact and frequent recurrence, the treatment of nail fungus on the hands and feet is a complex and lengthy process.
When does infection occur?
- In families with the general use of shoes, household items (rugs in the bathroom) and body care products (washcloths, manicure sets);
- When visiting swimming pools, showers in gyms and at enterprises, saunas and baths.
Causative agents of the disease
Effective treatment of nail fungus is possible only with the correct laboratory diagnosis of the pathogen. In almost 90% of cases, onychomycosis is caused by various types of dermatophyte. A specific species affects the corresponding parts of the body that are characteristic of it:
- nails of feet and hands, as well as any part of the skin;
- nail plates on the feet and the skin of the III-IV interdigital spaces, the arch of the foot, the upper third of the sole, the lateral surfaces of the toes.
In more rare cases, the disease is caused by other types of fungi - trichophytos, epidermophytos, much less often - yeast-like. Very rarely, onychomycosis can be caused by molds that affect the nails in the area of the first toes, mainly in people over 50.
Contributing factors
Favorable conditions for the introduction and development of infection:
- Damage to the nail plate and the skin around it. This often happens as a result of wearing tight shoes, cosmetic procedures.
- Fractures of the fingers and bones of the foot or hand.
- Swelling of the legs with heart disease, obliterating atherosclerosis of the lower extremities, varicose veins, Raynaud's disease (spasms of the arteries of the upper extremities).
- Endocrine diseases (especially diabetes mellitus).
- Pregnancy (due to hormonal changes and decreased immunity).
- Decreased general immunity.
- Congenital anomalies in the formation of the stratum corneum of the skin.
- Severe and long-term chronic diseases that reduce the body's defenses.
- Long-term treatment with corticosteroid drugs and antibiotics, systemic and other immune diseases.
The possibility of transmission of infection in the body itself by blood and lymph has already been proven.
Diagnostics of the onychomycosis
Diagnosis of a fungal infection is based on local and general clinical manifestations and laboratory research.
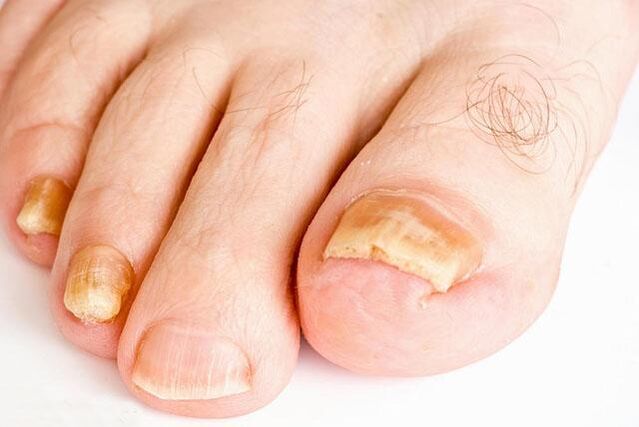
Clinical manifestations
Symptoms are very diverse and depend on the type and type of pathogen. Separately, the nails of the feet (80%) and hands can be affected; less common is the simultaneous defeat of the nails of the lower and upper extremities.
Depending on the nature of the change in the nail plate, 4 forms of damage are distinguished:
- Normotrophic- characterized by a yellowish coloration of the end edge of the nail plate. It becomes dull and thickened due to the epidermal stratum corneum (subungual hyperkeratosis). The shape of the affected nails does not change for a long time.
- Hypertrophic, in which the nail becomes yellowish and thickens, the edges are loosened. Transverse striation gradually appears. The nail plate becomes dirty gray and dull. In some cases, it (usually on the first toes) thickens, becomes long and curved like a bird's claw or beak (onychogryphosis).
- Atrophic- nails are dull, grayish or yellow. They change their shape, collapse at the end edge, partially exposing the bed. The latter is covered with loose layers of the stratum corneum.
- Onycholysis- detachment of the nail plate from the bed. With this form of fungal infection, the normal color remains only in the root area. The rest of the nail becomes thinner, separates from the bed, loses its luster and becomes yellowish or greyish-dirty.
Combined forms are often observed. The listed clinical manifestations are not specific for specific types of fungal lesions. They can also be in diseases not associated with fungi.
Some common manifestations are also possible: an allergic rash on the body, increased fatigue, and decreased appetite. They are explained by the ability of some types of dermatophytes to cause allergic restructuring of the body, and mold fungi - to release toxins, leading to chronic intoxication of the whole body.
Laboratory diagnostics
It consists in the collection of material (particles of layers of the epidermis, pieces of nails). The taken material is poured with a solution of caustic alkali, left for 24 hours at a temperature of about 20 degrees, after which it is examined under a microscope. This technique allows for differential diagnosis between fungal and non-fungal lesions. In the presence of a fungus, filaments of various thicknesses and shapes, groups of spores are visible under a microscope.
After that, the material is sown on a special nutrient medium for the growth of the pathogen, followed by identification of its type and determination for sensitivity to antimycotic drugs.
Treatment features
When choosing the methods of therapy, the form, type and extent of the lesion, the speed of nail growth, the general condition of the body and the side effects of the drugs used are taken into account, especially in the presence of concomitant diseases. Based on these principles, the treatment of toenail fungus, as well as on the hands, consists in a local or complex effect.
Local Impact Principles
It is possible if:
- the infection has not affected all the nails;
- the defeat of each of the infected nail plates is less than half of its area;
- the process is located only on the end and side sections of the plate without involving the root;
- there are contraindications to the use of systemic drugs.
Local drug treatment
It consists in using a cream, solution or nail polish containing substances that soften the nail plate. They also include drugs for the treatment of toenail (hand) fungus, which suppress the growth and development of infection:
You can pre-apply any preparations to soften the plate and remove it layer by layer, as in the first case, and then 2 times a day apply broad spectrum antifungal drugs in the form of creams or solutions. At the same time, it is necessary to rub them into the surrounding skin.
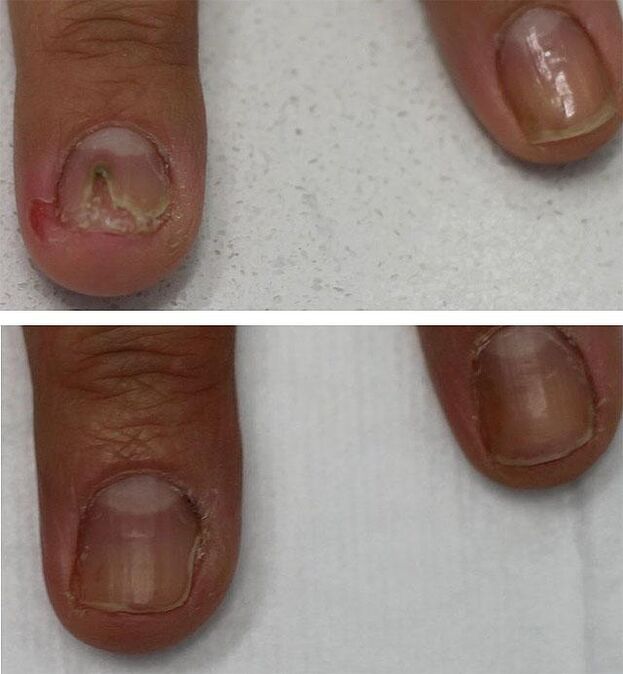
Medical hardware pedicure
A medical pedicure is used as an additional procedure (but not a treatment! ) That shortens the treatment time. Its essence is to use a router with an attachment in the form of a metal or diamond cutter. This device greatly facilitates the painless removal of a previously softened nail to its bed. The use of the hardware method is advisable when more than 60% of the area of the nail plate is damaged, but does not replace further drug treatment with antimycotic agents.
Surgery
In cases of severe forms of onychomycosis with severe deformation of the nail, it is sometimes removed surgically under general anesthesia or conduction anesthesia with further use of antifungal drugs. The main disadvantage of the method is damage to the nail bed, as a result of which the new grown plate lags behind it and has an irregular shape.
Laser treatment
This method consists in heating the nail with laser radiation in a short-pulse range to a temperature of 45-47 degrees, at which dermatophytes die. The procedure is most effective at the initial stages of nail damage without deformation. Depending on the severity, it is necessary to carry out from 1 to 8 sessions with an interval of 7 to 60 days. In severe lesions, local and systemic treatment should be carried out.
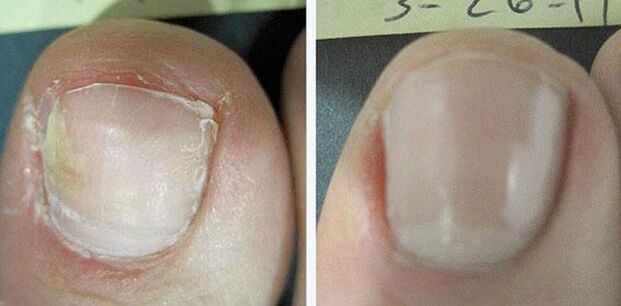
Systemic drug therapy
It is indicated for multiple lesions of the nails, involvement of the root in the process and in the absence of the effect of local exposure.
The most effective drugs for treating nail fungus are tablets. containing substances such as terbinafine, fluconazole, and others. They are prescribed in courses for 3-4 months, and remain in the body after the end of treatment for up to 9 months. The last two drugs, due to the toxic effect on the liver, are used much less frequently.
Systemic treatment is contraindicated in kidney and liver diseases. During pregnancy and lactation, only local treatment of 1-2 nails is possible, but it is better to refrain from this.
























